Benign Paroxysmal Positional Vertigo (BPPV)
Also known as: Benign Paroxysmal Positional Vertigo, BPPV, Positional Vertigo
DEFINITION
Benign Paroxysmal Positional Vertigo (BPPV) is one of the most prevalent causes of peripheral vestibular vertigo. It is characterized by sudden, brief attacks of a spinning sensation (vertigo) triggered by changes in the position of the head relative to gravity.
SYMPTOMS
The clinical presentation of BPPV typically includes:
- Intense rotational vertigo, usually lasting less than one minute.
- A persistent sense of instability or imbalance between attacks.
- Vegetative manifestations such as nausea and, in severe cases, vomiting.
- Positional nystagmus (involuntary rhythmic eye movements) synchronous with the vertigo attack.
When to see a doctor: Recurrent episodes of positional vertigo persisting for more than a few days require specialized clinical evaluation.
CAUSES AND PATHOGENESIS
In most cases, the exact cause of BPPV remains unknown (idiopathic form). However, several etiological factors are recognized:
- Head trauma: Even minor impacts can lead to the displacement of otoliths.
- Inner ear diseases: A history of vestibular neuritis, labyrinthitis, or Ménière's disease.
- Age-related changes: Degeneration of the macula in the saccule or utricle.
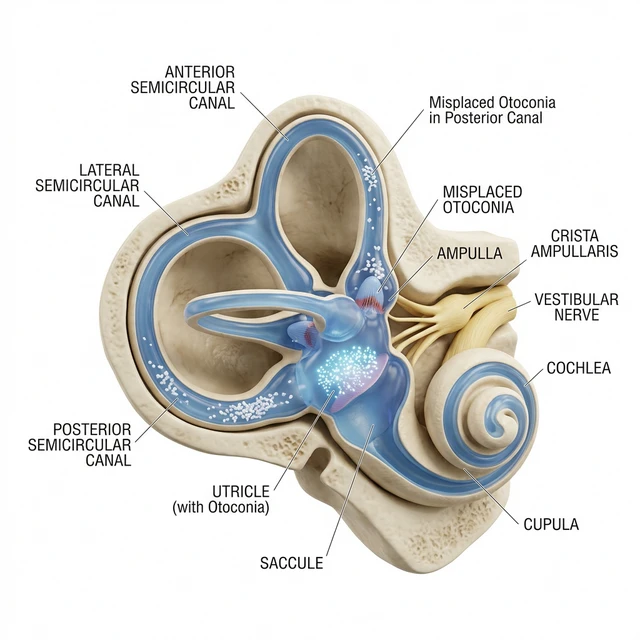
Pathogenesis: The underlying mechanism is canalithiasis — the displacement of microscopic calcium carbonate crystals (otoliths) from the vestibule into one of the semicircular canals (most often the posterior canal). As the head moves, these particles shift due to gravity, causing abnormal endolymph flow and stimulating receptors, which the brain interprets as a false signal of active rotation.
RISK FACTORS
The condition primarily manifests in patients over 50 years of age, with a higher prevalence among women. A history of head trauma, osteoporosis, and previous otoneurological disorders also increases the statistical risk of developing BPPV.
COMPLICATIONS
Extremely "benign" in nature, BPPV’s pronounced vestibular disturbance significantly increases the risk of falls and injuries (especially in elderly patients). It can also lead to the development of anxiety disorders, a fear of moving the head, and a significant reduction in quality of life.
PREPARING FOR YOUR APPOINTMENT
To optimize the diagnostic process, patients are advised to prepare:
- A timeline and detailed description of the attacks (triggering movements, exact duration).
- Information about any previous head trauma, infections, or ear surgeries.
- A complete list of all medications currently being taken.
TESTS AND DIAGNOSIS
Diagnosis is based on a characteristic medical history and clinical examination using specialized positional maneuvers. The gold standard for diagnosis is the Dix-Hallpike maneuver. To objectively visualize the induced nystagmus, the following are used:
- Electronystagmography (ENG) or Videonystagmography (VNG).
Additional imaging methods (such as Brain MRI) are used exclusively for differential diagnosis to rule out central causes (such as tumors or vascular disorders).
TREATMENTS AND DRUGS
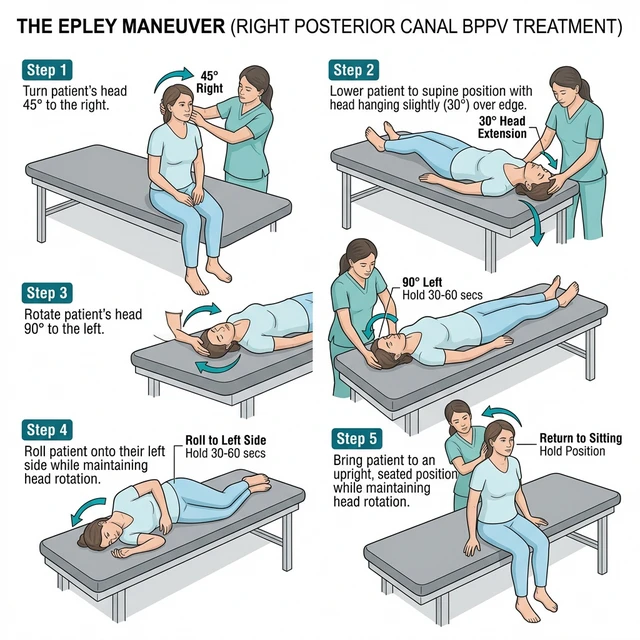
The primary and most effective treatment method for BPPV is the use of repositioning maneuvers. These are specialized therapeutic movements (such as the Epley, Semont, or Lempert maneuver) aimed at mechanically moving the otoliths out of the semicircular canals and back into the vestibule under the influence of gravity.
Pharmacological therapy does not affect the primary cause of the disease and should only be used if necessary for temporary relief of severe vegetative symptoms. Surgery is considered only in exceptional cases with persistent resistance to conservative therapy.
LIFESTYLE AND HOME REMEDIES
After performing a therapeutic repositioning maneuver, patients are advised to:
- Avoid sudden head movements or extreme head tilts.
- Immediately take a safe sitting or lying position if feeling signs of dizziness to avoid falling.
- If residual balance disturbances persist, strictly follow recommendations for performing rehabilitative gymnastics.
FAQ
What is BPPV?
Benign Paroxysmal Positional Vertigo (BPPV) is a common inner ear disorder that causes short but intense episodes of spinning (vertigo) in response to specific changes in head position.
Who is most commonly affected by BPPV?
It is most frequently diagnosed in women and individuals over the age of 50.
What are the primary symptoms of BPPV?
Key symptoms include sudden rotational vertigo, nausea, loss of balance, and involuntary eye movements (nystagmus).
How do doctors confirm the diagnosis?
Diagnosis is based on medical history and positional testing, such as the Dix-Hallpike maneuver. Specialists may also use electronystagmography (ENG) or videonystagmography (VNG) to assess eye movements.
What are repositioning maneuvers?
These are the primary treatments for BPPV (e.g., Epley or Semont maneuver). They involve a series of specific head and body movements aimed at moving crystals (otoliths) out of the semicircular canals and back into the vestibule of the ear via gravity.
When is vertigo considered an emergency?
Seek immediate medical attention if vertigo is accompanied by neurological signs such as muscle weakness, difficulty speaking, double vision, severe headache, or high fever.
Can BPPV return after treatment?
Yes, recurrence is possible. However, it can usually be successfully treated again with the appropriate repositioning maneuvers.
Are medications effective for BPPV?
Medications generally do not treat the underlying cause of BPPV. They may be used temporarily to relieve severe nausea, but repositioning maneuvers are the definitive therapy.
What role do "crystals" play in the inner ear?
These are otoliths (calcium carbonate crystals) that normally help detect gravity in the vestibule. In BPPV, they become dislodged and enter the semicircular canals, causing false stimulation of receptors when the head moves.
Is vestibular rehabilitation helpful?
Following a successful repositioning maneuver, a doctor may suggest specific vestibular rehabilitation exercises to help the brain more quickly regain optimal balance and labyrinth function.
Available in other languages
- pl Łagodne paroksyzmalne położeniowe zawroty głowy (BPPV)
- sv Godartad paroxysmal positionell vertigo (BPPV)
- no Benign paroksysmal posisjonsvertigo (BPPV)
- it Vertigine Posizionale Parossistica Benigna (VPPB)
- ru Доброкачественное пароксизмальное позиционное головокружение (ДППГ)
- pt Vertigem Posicional Paroxística Benigna (VPPB)
- uk Доброякісне пароксизмальне позиційне запаморочення (ДППЗ)
- hi बेनाइन पैरॉक्सिस्मल पोजिशनल वर्टिगो (BPPV)
- de Gutartiger paroxysmaler Lagerungsschwindel (BPPV)
- id Vertigo Posisi Paroksismal Jinak (BPPV)
- fr Vertige Positionnel Paroxystique Bénin (VPPB)
- es Vértigo Posicional Paroxístico Benigno (VPPB)
-
en Benign Paroxysmal Positional Vertigo (BPPV)
- tr İyi huylu paroksismal pozisyonel vertigo (BPPV)
